Three types of immobilisation are used for Achilles tendon rupture recovery: a plaster or fibreglass cast, a wedge-based walking boot (such as the Aircast AirSelect Elite or DonJoy Walker), or a hinged equinus boot (such as the VACOped). The UKSTAR trial — the largest RCT on this question — found that functional walking boots produce equivalent outcomes to traditional plaster casts. Current evidence suggests the rehabilitation protocol (how quickly weight-bearing is introduced, how the ankle angle progresses) matters more than which specific boot is used. Boot choice is made by your treating surgeon or physiotherapist. General information only — not medical advice.
Current evidence suggests that the rehabilitation protocol — how quickly weight-bearing is introduced, how the ankle angle is progressively adjusted, and the quality of physiotherapy — has a greater influence on outcomes than which specific immobilisation device is used. That said, there are meaningful biomechanical differences between boot types that are worth understanding, particularly as they may inform conversations with your treating clinician.
Does the Type of Boot You Wear Affect Achilles Rupture Recovery?
The primary goal of any immobilisation device following Achilles tendon rupture is to hold the ankle in a plantarflexed position — commonly referred to as equinus — so that the torn tendon ends are approximated (brought close together) and can heal at the correct length. If the tendon heals in a lengthened position, permanent calf weakness can result.
Research suggests that up to approximately 10mm of tendon lengthening is generally well tolerated, but beyond this threshold, clinically meaningful loss of plantarflexion power is reported in the literature. The degree to which different immobilisation devices achieve and maintain the required ankle angle is therefore clinically relevant — at least in theory.
What makes this topic more complex is that the biomechanical differences between boot types, while measurable and documented, have not yet been clearly shown to translate into different clinical outcomes in randomised controlled trials. This distinction — between biomechanical evidence and clinical outcome evidence — runs through this entire page and is important to understand.
What Are the Different Boots and Casts Used for Achilles Tendon Rupture?
Clinical literature and rehabilitation protocols describe three main immobilisation approaches for Achilles tendon rupture. Most patients encounter at least two of these during their recovery.
A non-removable plaster or fibreglass cast applied with the ankle held in plantarflexion. Historically the default treatment for Achilles tendon rupture. Still used in some protocols during the first one to two weeks post-injury or post-surgery to provide maximum protection while the tendon is at its most vulnerable. The cast is typically changed at intervals to progressively reduce plantarflexion toward neutral over six to eight weeks.
- Achieves true ankle plantarflexion (~56° tibiotalar angle)
- Cannot be removed — eliminates compliance risk
- Maximum tendon protection in acute phase
- Widely available in all clinical settings
- Non-removable — cannot shower normally
- Prolonged non-weight-bearing increases DVT risk
- Associated with greater calf muscle atrophy
- Ankle stiffness and gait abnormalities after removal
- Cannot be adjusted as healing progresses
A removable walking boot that uses stacked foam or rigid heel wedges to position the ankle in plantarflexion. The most widely used functional rehabilitation device in clinical practice worldwide. Wedges are progressively removed — typically one wedge every one to two weeks — to gradually bring the ankle toward neutral as the tendon heals. Allows early protected weight-bearing, which current evidence supports as beneficial compared to prolonged non-weight-bearing. Common examples of wedge-based walking boots used for Achilles rupture recovery include the Aircast AirSelect Elite (DJO), the DonJoy Walker, and the Össur Rebound Walker. The specific boot prescribed will depend on your clinician's preference and local availability.
- Allows early protected weight-bearing
- Removable — improves hygiene and sleep
- Widely available and generally lower cost
- Simple wedge adjustment — straightforward for patients
- Well-studied in major clinical trials
- Achieves less true ankle equinus than hinged boots (28° vs 48° tibiotalar angle)
- Equinus appearance partly from midfoot bending, not ankle joint
- Less tendon load reduction than posterior strut boots
- Gait asymmetry requires shoe leveller on opposite foot
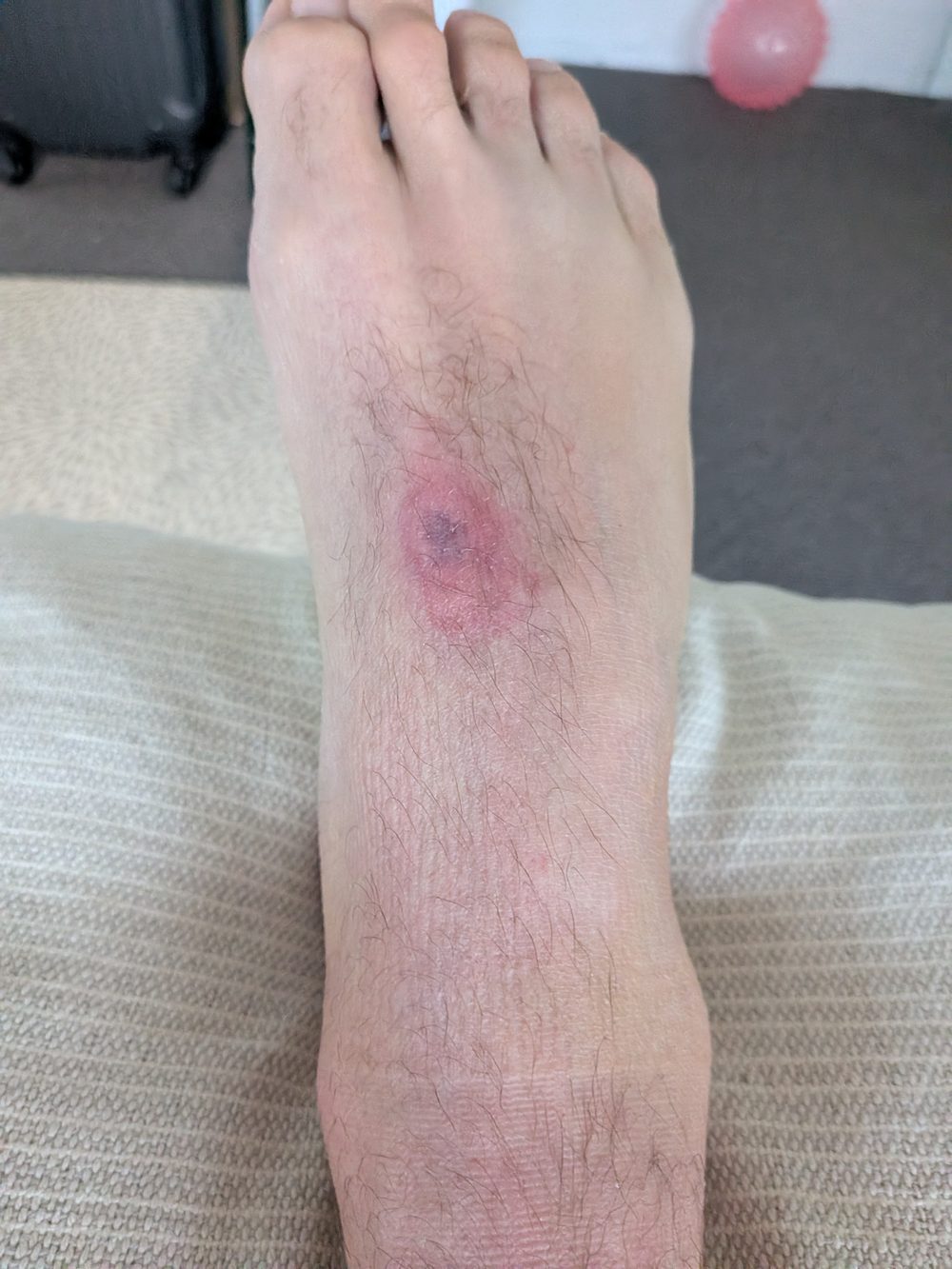
This pressure sore developed on the top of the foot during the first week of boot use — caused by a strap fitted too tightly. It is a common and largely avoidable complication.
When fitting a walking boot, straps should be firm enough to prevent the foot moving inside the boot, but you should be able to slide a finger under each strap. Check for any points of pressure or redness at the end of each day, particularly over bony prominences on the top of the foot. If a sore develops, contact your clinician — do not simply loosen all straps, as the foot moving inside the boot creates its own problems.
A removable boot featuring an articulating ankle hinge constrained by an adjustable posterior strut. The hinge allows precise control of ankle angle through a dial or adjustment mechanism, and can later be unlocked to permit a controlled range of motion as rehabilitation progresses. Achieves a greater degree of true ankle plantarflexion than wedge-based boots. Used as the boot of choice in several high-profile clinical protocols and referenced in major rehabilitation trials. The VACOped (OPED Medical) is the most clinically studied example of a hinged equinus boot for Achilles tendon rupture, and was used in the biomechanical comparison by Ellison et al. (2017). Other hinged equinus braces are available. Your treating clinician will select the most appropriate device.
- Achieves greater true ankle plantarflexion (48° vs 28° tibiotalar angle)
- Greater tendon load reduction (77% vs 60–68% for wedge boots)
- Precise angle adjustment via dial mechanism
- Later ROM capability may reduce muscle atrophy
- Used in major clinical protocols including SMART and LAMP
- Significantly higher cost than wedge-based boots
- Heavier and bulkier — some patients find gait more difficult
- More complex adjustment — requires careful clinician instruction
- Less widely available, particularly in public hospital settings
- No RCT evidence of superior clinical outcomes vs wedge boots
Why Does the Equinus Ankle Angle Matter — and Does Your Boot Actually Achieve It?
One of the most clinically significant findings in the boot comparison literature comes from a study by Ellison et al. (2017), published in the Journal of Foot and Ankle Surgery. Using weight-bearing radiographs, the study compared the true ankle angle achieved by a fixed-angle walking boot with wedges versus an adjustable equinus-corrected brace — and found a meaningful difference that is not visible from the outside.
Mean tibiotalar angle. True ankle equinus. The reference standard — all angulation comes from the ankle joint itself.
Mean tibiotalar angle. Significantly less than cast equinus. Ellison et al. found the equinus appearance in wedge boots is produced partly through midfoot bending, not true ankle plantarflexion.
Mean tibiotalar angle. Closer to cast equinus. All angulation comes from the ankle joint, not the midfoot. Authors expressed caution about wedge boot use on this basis.
The clinical significance of this finding is that a wedge-based boot may allow more tendon lengthening than it appears to, because the foot is bending at the midfoot rather than plantarflexing fully at the ankle joint. The theoretical concern is that tendons healing in a more lengthened position may result in weaker calf muscle function long-term.
Despite the measurable difference in ankle angle between boot types, no randomised controlled trial has yet demonstrated that this difference translates into different functional outcomes, re-rupture rates, or tendon length at follow-up. The Ellison et al. study authors themselves noted that "the clinical relevance of this remains uncertain." This is an important distinction — the theoretical concern is real and well-reasoned, but the clinical evidence to confirm it does not yet exist.
How Much Do Different Boots Reduce Load on the Healing Achilles Tendon?
A biomechanical study published in Foot and Ankle Orthopaedics (2022) measured Achilles tendon loading during walking in three different immobilising boots compared to normal walking in shoes. The study found that all boots significantly reduced tendon loading, but there were meaningful differences between boot constructions.
Approximate relative tendon loading as percentage of normal walking. Bars represent residual loading (lower = better protection). Source: Foot and Ankle Orthopaedics 2022 (PMC9661566).
The study found that wedge-based boots reduced tendon loading by approximately 60–68% compared to normal walking. The hinged posterior strut boot reduced loading by approximately 77%. The authors noted that only the posterior strut boot reduced tendon loading to levels below the threshold estimated for surgical repair — suggesting potentially superior protection in the early healing phase.
Greater tendon load reduction is biomechanically advantageous in theory, particularly in the early weeks when the healing tendon is weakest. However, as with the equinus angle difference, no RCT has yet demonstrated that this biomechanical difference translates into measurably better clinical outcomes. Both boot types are used successfully in major clinical trials with good outcomes.
Is a Walking Boot as Good as a Plaster Cast for Achilles Rupture Recovery?
The question of whether a functional walking boot produces equivalent outcomes to traditional plaster casting was definitively addressed by the UKSTAR trial — the largest and most rigorous RCT on this specific question.
A multicentre pragmatic RCT across 39 NHS hospitals in the UK. 540 adults receiving non-operative treatment for Achilles tendon rupture were randomised to plaster cast or functional walking boot for 8 weeks. Primary outcome was ATRS at 9 months. Funded by UK National Institute for Health Research.
The UKSTAR trial concluded that early weight-bearing in a functional brace provides similar outcomes to traditional plaster casting at 9 months and is a safe treatment for non-operative Achilles tendon rupture. The functional brace showed an early advantage at 8 weeks — likely reflecting the benefit of earlier mobility and weight-bearing — which was not sustained at later follow-up points. Cost was similar between groups.
This finding is now reflected in most clinical guidelines, which support functional walking boot rehabilitation as a safe and effective alternative to plaster casting for non-operatively managed Achilles tendon ruptures.
Is a VACOped Better Than an Aircast or Wedge Boot for Achilles Recovery?
The question patients most frequently ask — and the one the internet most frequently gets wrong — is whether the type of walking boot matters. The evidence-based answer, as of the most recent published literature, is as follows.
"There are no randomised controlled trials directly comparing hinged equinus boots with wedge-based walking boots on clinical outcomes in Achilles tendon rupture."
This is the honest state of the literature. The biomechanical evidence — ankle angle measurements, tendon loading studies — clearly demonstrates that hinged posterior strut boots achieve greater true ankle plantarflexion and reduce tendon loading more effectively than wedge-based boots. These are real, measurable, and clinically plausible differences.
However, the leap from biomechanical difference to clinical outcome difference has not been demonstrated in a randomised trial. Both boot types are used in major clinical protocols with good outcomes. The SMART protocol, which uses a hinged equinus boot, reported a 1.1% re-rupture rate across 211 patients. The LAMP protocol, also using a hinged boot, achieved a 2% re-rupture rate across 442 patients. But without a direct randomised comparison with wedge boot protocols under equivalent conditions, attributing these outcomes to boot type rather than protocol quality is not possible.
What the literature does clearly support is that the overall rehabilitation protocol — early weight-bearing, progressive angle adjustment, physiotherapy quality, and patient adherence — is a more powerful determinant of outcome than boot type. A wedge-based boot used within a well-structured, closely supervised protocol is likely to produce better outcomes than a hinged boot used inconsistently or without proper physiotherapy support.
How Do Plaster Cast, Wedge Boot and Hinged Boot Compare for Achilles Rupture?
The following table summarises the key differences between the three immobilisation types based on published literature. Clinical outcome comparisons between boot types are based on biomechanical studies and observational data, not direct RCT evidence.
| Feature | Plaster Cast | Wedge Boot | Hinged Equinus Boot |
|---|---|---|---|
True ankle equinus |
~56° (reference) | ~28° — partly via midfoot compensation | ~48° — true ankle angle |
Tendon load reduction |
Near complete (non-WB) | ~60–68% vs normal walking | ~77% vs normal walking |
Early weight-bearing |
No — typically 6 wks NWB | Yes — immediate or early | Yes — immediate or early |
Removable |
No | Yes | Yes |
RCT evidence vs cast |
Reference standard | Yes — UKSTAR 2020 (n=540): equivalent outcomes at 9 months | Indirect — used in trials but not directly compared to cast in large RCT |
RCT vs other boot type |
N/A | None published | None published |
Cost (approximate) |
Low — clinical material | Lower — ~A$150–250 | Higher — ~A$400–600 |
Availability |
Universal | Wide — most hospitals | Variable — more common in private settings |
What Should I Ask My Surgeon or Physio About My Boot or Cast Choice?
The following questions may help readers have a more informed conversation with their treating orthopaedic surgeon, sports medicine physician, or physiotherapist about their immobilisation approach.
- Which type of boot will I be fitted with, and why is that the preferred choice in my case?
- What is the specific angle protocol — at what intervals will the angle be adjusted, and by how much?
- When am I expected to commence full weight-bearing, and what should I do if it is painful?
- Is a plaster cast being used initially, and if so, for how long before I transition to a boot?
- Should I be using a shoe leveller on my other foot to correct gait asymmetry while in the boot?
- Should I be removing the boot to sleep, and if so, how should I position my ankle overnight?
- What are the signs that I should contact you — increased pain, swelling, or changes in the boot fit?
What Does the Evidence Actually Say About Boot Choice for Achilles Rupture?
Based on current peer-reviewed evidence, the following conclusions are supported by the literature:
- Functional walking boot rehabilitation produces equivalent outcomes to plaster casting at 9 months and is considered a safe, evidence-supported approach for non-operative Achilles rupture management — confirmed by the UKSTAR RCT (540 patients, The Lancet 2020)
- Hinged equinus boots achieve greater true ankle plantarflexion and greater tendon load reduction than wedge-based boots — these are real biomechanical differences confirmed in published studies
- No randomised controlled trial has yet demonstrated that hinged equinus boots produce better clinical outcomes than wedge-based boots — the biomechanical advantage has not been translated into proven clinical benefit
- Protocol adherence — how consistently the patient follows the prescribed angle adjustments and weight-bearing schedule — is likely to be a more important determinant of outcome than which boot type is used
- The boot provided in your clinical setting, used correctly within a well-supervised rehabilitation protocol, is the most important factor — not the brand or category of boot
- Questions about boot type are worth raising with your treating clinician, particularly in private settings where device choice may be more flexible
This page provides general health information only. It is compiled from peer-reviewed medical literature and published clinical guidelines and is intended to help readers understand the evidence base for immobilisation approaches used in Achilles tendon rupture recovery.
The content on this page does not constitute medical advice and does not create a clinical or professional relationship between the reader and this website or its authors. The type of immobilisation used in your treatment is a clinical decision that should be made in consultation with your treating healthcare professional.
Individual clinical circumstances vary significantly. Always follow the specific immobilisation protocol prescribed by your treating clinician, and contact them if you have concerns about your device or your recovery progress.
Some links on this site are affiliate links. If you purchase a product through these links, this site may earn a small commission at no additional cost to you. Affiliate relationships do not influence the health information provided on this or any other page.